THE DIAGNOSTIC DILEMMA: Are CT Scans Driving a Hidden Cancer Spike?
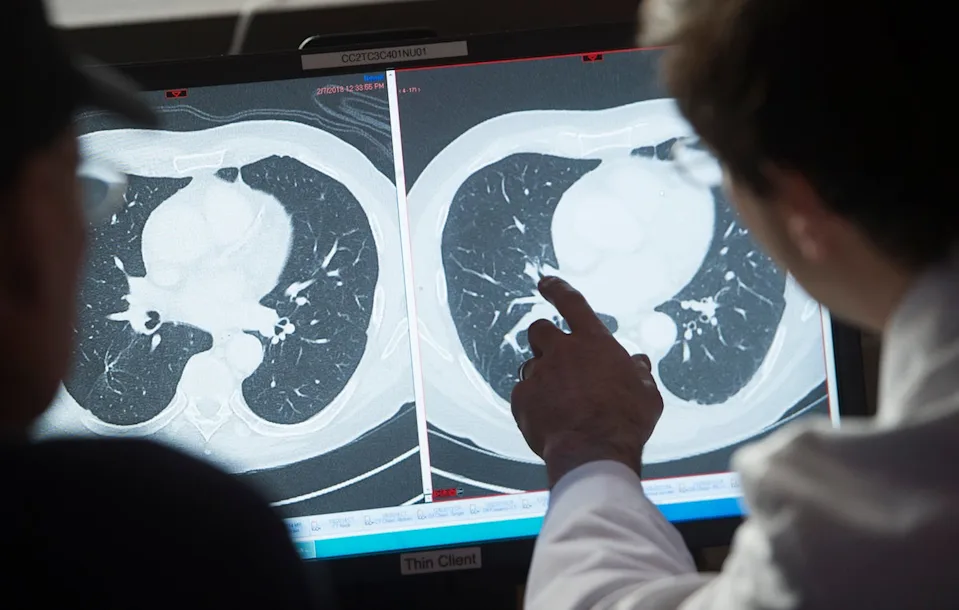
WASHINGTON, D.C. — For decades, the CT scan has been the gold standard for rapid diagnosis, from detecting internal bleeding after a car crash to identifying early-stage tumors. However, a sobering body of research has begun to quantify the invisible cost of this medical revolution: a significant, long-term increase in cancer risk associated with cumulative radiation exposure.
The 103,000 Estimate
Recent large-scale longitudinal studies—including a prominent 2023 analysis published in Nature Medicine—have sent shockwaves through the medical community. The data suggests that as CT scan usage has skyrocketed, so has the incidence of radiation-induced cancers. Researchers estimated that roughly 103,000 cases of cancer in the studied population could be attributed to the cumulative radiation dose received from CT imaging.
While these numbers are projections based on statistical models, they highlight a reality that has long been suspected: medical radiation is not benign.
The “Radiation Debt” Mechanism
Why do these scans carry risk? Unlike an X-ray, which is a low-dose, one-dimensional image, a CT scan takes hundreds of X-ray images from different angles to create a detailed, 3D cross-section.
Cumulative Exposure: The danger isn’t necessarily one single scan, but the “stacking” of radiation doses over a lifetime.
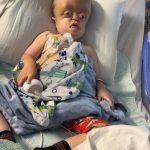
The Vulnerability Window: Studies show that the risk is particularly pronounced in younger patients (children and young adults), whose rapidly dividing cells are more susceptible to radiation-induced DNA mutations.
The “Unnecessary” Gap: Estimates suggest that a significant percentage of CT scans are “potentially avoidable”—ordered for minor injuries or conditions where clinical observation or ultrasound (which uses no ionizing radiation) would have been equally effective.
The ALARA Principle
The medical community is not advocating for an end to CT scans; they are advocating for the ALARA principle (As Low As Reasonably Achievable). This approach focuses on:
Dose Optimization: Using advanced software to adjust the radiation dose based on the patient’s size and the specific clinical need, effectively “dialing down” the radiation without losing image quality.
Clinical Justification: Forcing a stricter standard on why a scan is being ordered. Is it a “defensive medicine” practice to avoid a lawsuit, or is it truly necessary for treatment?
Alternative Imaging: Choosing MRI or ultrasound whenever possible, as these technologies do not use ionizing radiation.
The Path Forward
The challenge for 2026 and beyond is a cultural shift in medicine. Doctors must balance the immediate benefit of a clear diagnosis against the long-term statistical risk to the patient. We are entering an era of “Precision Imaging,” where the focus is moving away from more data toward better, safer data.