THE ARTIFICIAL WOMB: Redefining the “Micro-Preemie” Frontier
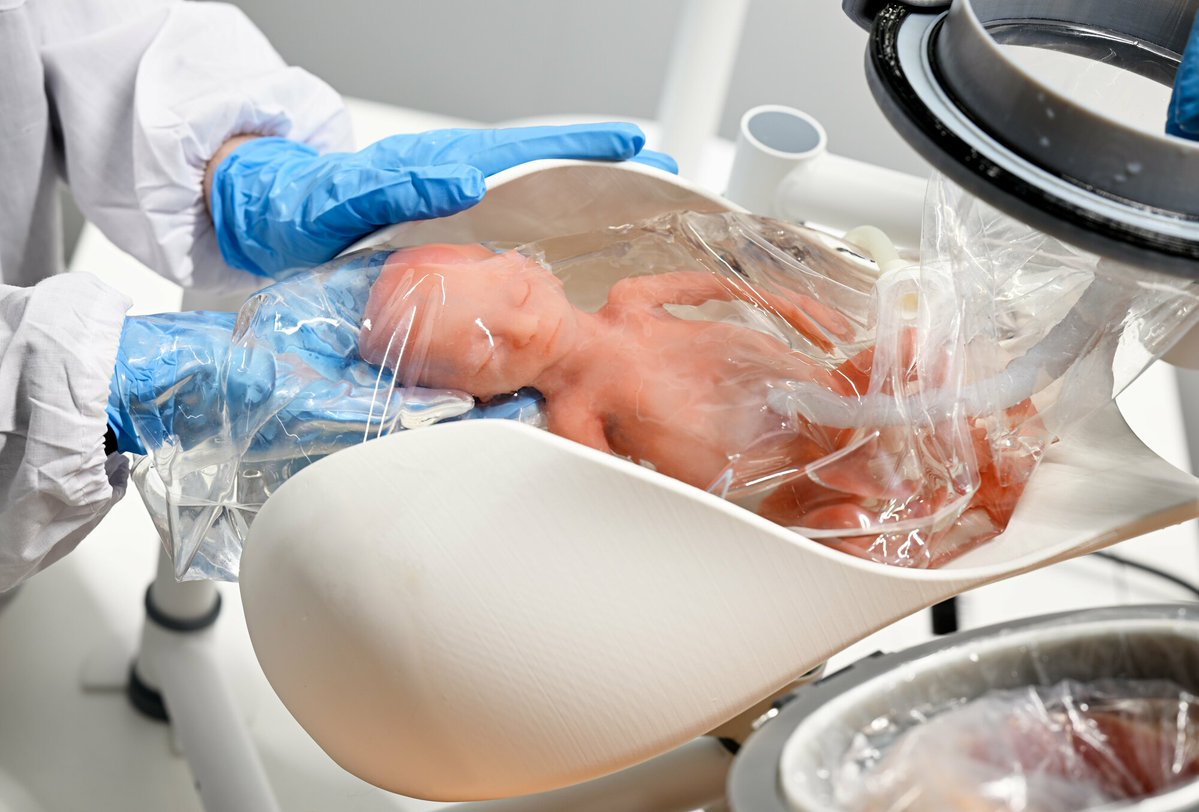
The Dutch “Perinatal Life Support” (PLS) concept, spearheaded by entities like the one you’ve described, is essentially a high-tech bridge. It recognizes that we cannot “fix” a 22-week-old lung; we can only protect it.
1. The Fluid Environment
The use of synthetic amniotic fluid is the key. In the mother’s womb, the fetus is suspended in fluid, which provides a weightless environment that prevents skeletal deformation and, crucially, keeps the lungs collapsed and “at rest” while they develop.
2. The Placental Bypass
The most technically daunting aspect is replacing the placenta. In a natural pregnancy, the placenta handles gas exchange ($O_2$ and $CO_2$) and nutrient delivery without the fetus ever needing to expand its lungs. This system replicates that by connecting an “artificial placenta” to the umbilical cord.
3. The Ethical “Bio-Boundary”
You hit on the most critical point: the ethical frontier. If we can successfully sustain a fetus outside the womb at 22 weeks, the legal and ethical definition of “viability” becomes incredibly fluid. Does this technology turn the NICU into a second trimester of pregnancy? That is exactly why the FDA and medical ethics boards are moving with extreme caution. We are entering a space where the biological start of life is being fundamentally redefined.











